Abstract
Background and aims
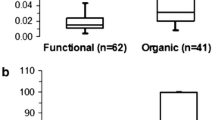
Calprotectin and lactoferrin are specific neutrophil-derived proteins, which can be measured in the feces because they are released by cells in inflammatory conditions. We evaluated the efficacy of calprotectin and lactoferrin in detecting organic disease as assessed by colonoscopy.
Methods
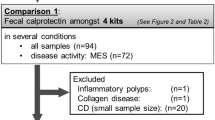
The study comprised 144 patients undergoing colonoscopy for lower gastrointestinal symptoms (abdominal pain, altered bowel habits, and bloody stools) (67), or inflammatory bowel disease activity, or surveillance for dysplasia (77). A single stool sample was assayed for calprotectin and lactoferrin. The proportion of patients correctly diagnosed with each test and the relationship with endoscopic and histological findings were measured.
Results
Fecal excretion of calprotectin significantly correlated with the finding of colonic inflammation at endoscopy, both in ulcerative colitis and in Crohn’s disease (p<0,001 and p<0,008, respectively), while lactoferrin excretion significantly correlated with histological inflammation (p=0.001 and p=0.009 respectively). Recommended cut-off values need to be adjusted in the inflammatory bowel disease group. Overall sensitivity, specificity, positive predictive value, and diagnostic efficacy were 78, 83, 86, and 80% for calprotectin and 80, 85, 87, and 81% for lactoferrin, respectively.
Conclusions
Fecal calprotectin and lactoferrin appear to be equally recommendable as inflammatory disease markers in patients with lower gastrointestinal symptoms. Both tests are needed to accurately discriminate activity in inflammatory bowel disease patients.




Similar content being viewed by others
References
Poullis A, Foster R, Mendall MA, Fagerhol MK (2003) Emerging role of calprotectin in gastroenterology. J Gastroenterol Hepatol 18(7):756–762
Kane SV, Sandborn WJ, Rufo PA, Zholudev A, Boone J, Lyerly D, Camilleri M, Hanauer SB (2003) Fecal lactoferrin is a sensitive and specific marker in identifying intestinal inflammation. Am J Gastroenterol 98(6):1309–1314
Guerrant RL, Araujo V, Soares E, Kotloff K, Lima AA, Cooper WH, Lee AG (1992) Measurement of fecal lactoferrin as a marker of fecal leukocytes. J Clin Microbiol 30(5):1238–1242
Martins CA, Fonteles MG, Barrett LJ, Guerrant RL (1995) Correlation of lactoferrin with neutrophilic inflammation in body fluids. Clin Diagn Lab Immunol 2(6):763–765
Sugi K, Saitoh O, Hirata I, Katsu K (1996) Fecal lactoferrin as a marker for disease activity in inflammatory bowel disease: comparison with other neutrophil-derived proteins. Am J Gastroenterol 91(5):927–934
Voganatsi A, Panyutich A, Miyasaki KT, Murthy RK (2001) Mechanism of extracellular release of human neutrophil calprotectin complex. J Leukoc Biol 70:130–134
Kayazawa M, Saitoh O, Kojima K, Nakagawa K, Tanaka S, Tabata K, Matsuse R, Uchida K, Hoshimoto M, Hirata I, Katsu K (2002) Lactoferrin in whole gut lavage fluid as a marker for disease activity in inflammatory bowel disease: comparison with other neutrophil-derived proteins. Am J Gastroenterol 97(2):360–369
Roseth AG, Fagerhol MK, Aadland E, Schjonsby H (1992) Assessment of the neutrophil dominating protein calprotectin in feces. A methodologic study. Scand J Gastroenterol 27(9):793–798
Fine KD, Ogunji F, George J, Niehaus MD, Guerrant RL (1998) Utility of a rapid fecal latex agglutination test detecting the neutrophil protein, lactoferrin, for diagnosing inflammatory causes of chronic diarrhea. Am J Gastroenterol 93(8):1300–1305
Gaya DR, Lyon TDB, Duncan A, Neilly JB, Han S, Howell J, Liddell C, Stanley AJ, Morris AJ, Mackenzie JF (2005) Fecal calprotectin in the assessment of Crohn’s disease activity. Q J Med 98:435–441
Summerton CB, Longlands MG, Wiener K, Shreeve DR (2002) Faecal calprotectin: a marker of inflammation throughout the intestinal tract. Eur J Gastroenterol Hepatol 14(8):841–845
Saitoh O, Kojima K, Kayazawa M, Sugi K, Tanaka S, Nakagawa K, Teranishi T, Matsuse R, Uchida K, Morikawa H, Hirata I, Katsu K (2000) Comparison of tests for fecal lactoferrin and fecal occult blood for colorectal diseases: a prospective pilot study. Intern Med 39(10):778–782
Silberer H, Kuppers B, Mickisch O, Baniewicz W, Drescher M, Traber L, Kempf A, Schmidt-Gayk H (2005) Fecal leukocyte proteins in inflammatory bowel disease and irritable bowel syndrome. Clin Lab 51(3–4):117–126
Langhorst J, Elsenbruch S, Mueller T, Rueffer A, Spahn G, Michalsen A, Dobos GJ (2005) Comparison of 4 neutrophil-derived proteins in feces as indicators of disease activity in ulcerative colitis. Inflamm Bowel Dis 11(12):1085–1091
Larsen A, Hovdenak N, Karlsdottir A, Wentzel-Larsen T, Dahl O, Fagerhol MK (2004) Faecal calprotectin and lactoferrin as markers of acute radiation proctitis: a pilot study of eight stool markers. Scand J Gastroenterol 30:1113–1118
Schroeder KW, Tremaine WJ, Ilstrup DM (1987) Coated oral 5-aminosalicylic acid therapy for mildly to moderately active ulcerative colitis. N Engl J Med 317:1625–1629
Floren CH, Benton C, Willen R (1987) Histological and colonoscopy assessment of disease extension in ulcerative colitis. Scand J Gastroenterol 22:459–462
Daperno M, D’Haens G, Van Assche G, Baert F, Bulois P, Maunoury V, Sostegni R, Rocca R, Pera A, Gevers A, Mary JY, Colombel JF, Rutgeerts P (2004) Development and validation of a new, simplified endoscopic activity score for Crohn’s disease: the SES-CD. Gastrointest Endosc 60:505–512
Fazio VW, Marchetti F, Church JM, Goldblum JR, Lavery C, Hull TL, Milsom JW, Strong SA, Oakley JR, Secic M (1996) Effect of resection margins on the recurrence of Crohn’s disease in the small bowel. Ann Surg 224:563–567
Limburg PJ, Ahlquist DA, Sandborn WJ, Mahoney DW, Devens ME, Harrington JJ, Zinsmeister AR (2000) Fecal calprotectin levels predict colorectal inflammation among patients with chronic diarrhea referred for colonoscopy. Am J Gastroenterol 95(10):2831–2837
Carroccio A, Iacono G, Cottone M, Di Prima L, Cartabellotta F, Cavataio F, Scalici C, Montalto G, Di Fede G, Rini G, Notarbartolo A, Averna MR (2003) Diagnostic accuracy of fecal calprotectin assay in distinguishing organic causes of chronic diarrhea from irritable bowel syndrome: a prospective study in adults and children. Clin Chem 49:861–867
Kapel N (2004) Faecal inflammatory markers in nutrition and digestive diseases in children. Arch Pediatr 11(5):403–405
Roseth AG, Schmidt PN, Fagerhol MK (1999) Correlation between faecal excretion of indium-111-labelled granulocytes and calprotectin, a granulocyte marker protein, in patients with inflammatory bowel disease. Scand J Gastroenterol 34(1):50–54
Braegger CP, Nicholls S, Murch SH, Stephens S, MacDonald TT (1992) Tumour necrosis factor alpha in stool as a marker of intestinal inflammation. Lancet 339:89–91
Tibble J, Sigthorsson G, Foster R, Sherwood R, Fagerhol M, Bjarnason I (2001) Faecal calprotectin and faecal occult blood tests in the diagnosis of colorectal carcinoma and adenoma. Gut 49(3):402–408
Kristjansson J, Armbruster CH, Ugstad M, Kriwanek S, Nygaard K, Ton H, Fuglerud P (2001) Fecal excretion of calprotectin in colorectal cancer: relationship to tumor characteristics. Scand J Gastroenterol 36(2):202–207
Roseth AG, Kristjansson J, Fagerhol MK, Schjonsby H, Aadland E, Nygaard K, Roald B (1993) Faecal calprotectin: a novel test for the diagnosis of colorectal cancer? Scand J Gastroenterol 28(12):1073–1076
Poullis A, Foster R, Shetty A, Fagerhol MK, Mendal MM (2004) Bowel inflammation as measured by fecal calprotectin: a link between lifestyle factors and colorectal cancer risk. Cancer Epidemiol Biomark Prev 13:279–284
Kronborg O, Ugstad M, Fuglerud P, Johne B, Hardcastle J, Scholefield JH, Vellacott K, Moshakis V, Reynolds JR (2000) Faecal calprotectin levels in a high risk population for colorectal neoplasia. Gut 46(6):795–800
Buderus S, Boone J, Lyerly D, Lentze MJ (2004) Fecal lactoferrin: a new parameter to monitor infliximab therapy. Dig Dis Sci 49(6):1036–1039
Roseth AG, Aadland E, Jahnsen J, Raknerud N (1997) Assessment of disease activity in ulcerative colitis by faecal calprotectin, a novel granulocyte marker protein. Digestion 58(2):176–180
Hanai H, Takeuchi K, Iida T, Kashiwagi N, Saniabadi AR, Matsushita I, Sato Y, Kasuga N, Nakamura T (2004) Relationship between fecal calprotectin, intestinal inflammation, and peripheral blood neutrophils in patients with active ulcerative colitis. Dig Dis Sci 49(9):1438–1443
Tibble JA, Sighthorsson G, Bridger S, Fagerhol MK, Bjarnason I (2000) Surrogate markers on intestinal inflammation are predictive of relapse in patients with inflammatory bowel disease. Gastroenterology 119:15–22
Costa F, Mumolo MG, Ceccarelli L, Bellini M, Romano MR, Sterpi C, Ricchiuti A, Marchi S, Bottai M (2005) Calprotectin is a strong predictive marker of relapse in ulcerative colitis than in Crohn’s disease. Gut 54:364–368
Acknowledgements
Dr. R. D’Incà and Dr. E. Dal Pont contributed equally to this work. This is supported in part by a grant from MIUR ex 40% 2004 (2004063577_004).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
D’Incà, R., Dal Pont, E., Di Leo, V. et al. Calprotectin and lactoferrin in the assessment of intestinal inflammation and organic disease. Int J Colorectal Dis 22, 429–437 (2007). https://doi.org/10.1007/s00384-006-0159-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-006-0159-9