Article Text
Abstract
A 62-year-old man presented to the emergency department with 5 weeks of worsening lower abdominal pain associated with watery diarrhoea, vomiting and 10% loss of body weight. He had recently experienced night blindness.
There was no history of foreign travel. His past medical history included hypertension, sickle cell trait and type 2 diabetes well controlled on metformin. He had not been prescribed any recent steroids and denied significant alcohol intake.
On examination, he had a tachycardia at 110 bpm and was afebrile and normotensive. He was malnourished with pedal pitting oedema extending to both knees. His abdomen was soft but distended and diffusely tender.
Blood tests showed a serum albumin of 12 g/L. Stool samples were negative. HIV testing was negative, and immunoglobulin levels were normal.
CT of the abdomen showed thickened, hyperenhancing jejunal loops with diffuse mesenteric inflammatory fat stranding and enlarged mesenteric lymph nodes. Colonoscopy was unremarkable.
Enteroscopy showed granular oedematous mucosa and extensive, deep ulcerations. Jejunal biopsies were obtained. Microscopy samples were negative for tuberculosis (TB) culture.
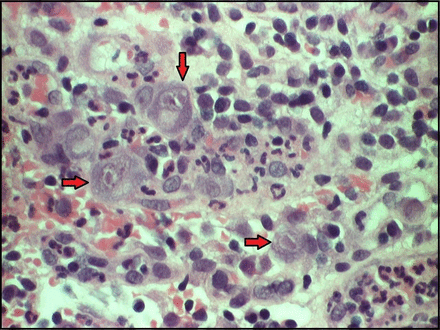
Histology revealed inflamed and ulcerated small bowel mucosa with plump endothelial cells with the appearance below. There were no granulomata (figures 1 and 2).
Endoscopic examination of the jejunum.
Plump endothelial cells seen on microscopy.
Question What is the differential diagnosis?
- small bowel disease
- colonoscopy
- enteric infections
- antiviral therapy
Statistics from Altmetric.com
Footnotes
Contributors Conception and design of study: GAS, JC. Acquisition of data: GAS, JC, JO’D. Analysis and/or interpretation of data: GAS, EL. Drafting the manuscript: GAS, JC, BW, JO’D. Revising the manuscript critically for important intellectual content: GAS, BW, JO’D. Approval of the version of the manuscript to be published: GAS, JC, BW, JO’D, EL.
Funding Funding provided by University Hospital Lewisham Gastroenterology Department Research Fund.
Competing interests None declared.
Patient consent Obtained.
Provenance and peer review Not commissioned; internally peer reviewed.
Collaborators Suzanne Donnelly, David Reffitt, David Dewar.